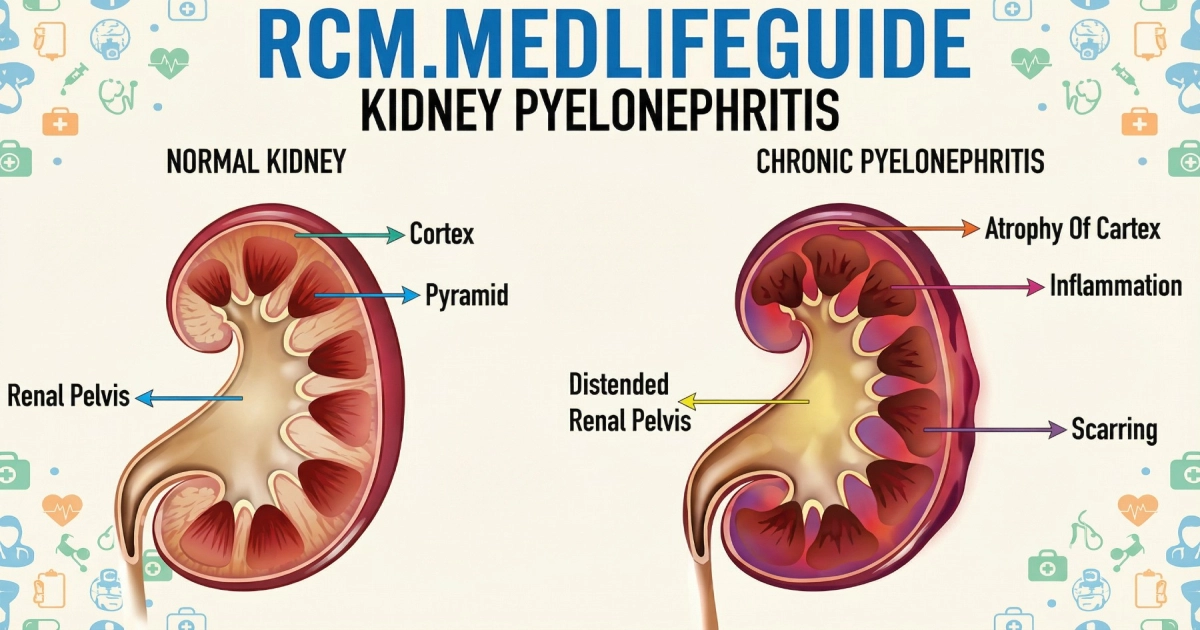
A kidney infection, also called pyelonephritis, is a serious type of urinary tract infection that moves beyond the bladder and into one or both kidneys. It usually starts as a lower UTI and climbs up the urinary tract, carried with the urine.
Research shows that kidney infections cause high fever
A kidney infection, also called pyelonephritis, is a serious type of urinary tract infection that moves beyond the bladder and into one or both kidneys. It usually starts as a lower UTI and climbs up the urinary tract, carried with the urine.
Research shows that kidney infections cause high fever, chills, pain in the side or lower back, and feeling extremely unwell far more than a simple bladder infection does.[1] Doctors treat it with an antibiotic course and close follow up because a kidney infection can lead to kidney damage, sepsis, and even kidney failure when someone delays care.[2]
If you feel like you have the flu plus UTI symptoms, do not wait. That combination usually signals a kidney infection rather than a harmless UTI.
Quick summary
Key points at a glance
- A kidney infection sits higher in the urinary tract than a standard UTI and attacks the kidney tissue itself.
- The main symptoms of a kidney infection include fever over 38°C / 100.4°F, chills, side or lower back pain, nausea, and burning or frequent urination.
- The common cause is bacteria from the gut, especially E. coli, that start in the bladder and then reach the kidneys.
- Diabetes, chronic kidney disease, kidney stone, high blood pressure, pregnancy, and a weakened immune system make it easier for bacteria to spread and increase the risk of complications.
- Untreated infections can lead to permanent kidney damage, blood infection, and kidney failure.
- Doctors confirm the diagnosis with a history, physical exam, urine tests, sometimes blood tests, and imaging.
- Treatment relies on the right antibiotic, hydration, and rest; severe cases need hospital care and IV drugs.
- You help prevent future kidney infections when you drink plenty of water, pee regularly, treat UTIs early, and wipe from front to back after using the toilet.
- Pregnant women and people with chronic conditions should call a doctor as soon as they suspect a UTI, not after days of waiting.
If you read nothing else, remember this:
Flu‑like symptoms plus UTI symptoms equal a medical problem that needs attention now, not tomorrow.
1. Why kidney infections deserve serious attention
Picture this.
Someone feels burning when they pee. They shrug and think, “Just a regular UTI. I’ll wait it out.” Two days later, they get hit with intense chills, sharp pain in their side, and a fever that sends them to bed.
That story shows how quickly a urinary tract infection can turn into pyelonephritis, a full kidney infection.
A kidney infection affects the kidney tissue itself, not just the bladder. Because kidneys filter the blood, any infection there sits one step away from the bloodstream. That is why infections in the kidneys run a higher risk of serious complications than a low UTI.
You want three things from a guide like this:
- Clarity – to know if your symptoms match a kidney problem.
- An action plan – what to do today if you suspect an infection.
- Long term protection – habits that protect your kidneys for years.
This article covers all three, with evidence, real‑world examples, and step‑by‑step advice you can follow.
2. Understanding kidney infections inside the urinary tract
How the urinary tract works
The urinary tract has four main parts:
- Kidneys – filter the blood, remove waste, and create urine.
- Ureters – thin tubes that carry urine from each kidney to the bladder.
- Bladder – stores urine.
- Urethra – the outlet that allows urine to leave the body.
Healthy kidneys act like ultra‑fine filters. They pull waste and extra fluid from the blood and send it out as urine. Steady urine flow helps flush out germs before they climb upward.
From bladder infection to kidney infection
Most kidney infections start low, as a bladder infection. Here is the usual chain:
- Bacteria enter through the urethra.
- They multiply in the bladder and create a urinary tract infection.
- If no one treats that UTI, bacteria continue traveling up the ureters.
- Bacteria reach the kidneys and trigger pyelonephritis.
E. coli from the gut causes the majority of UTIs and kidney infections in otherwise healthy people.[3] A shorter urethra and its proximity to the anus mean women are more likely to get these infections.
Strong urine flow and frequent emptying interrupt this chain. When you drink plenty of water and pee regularly, you physically wash out a significant load of bacteria before they gain a foothold.
3. Symptoms of a kidney infection: how to tell it is more than a UTI
Classic symptoms
When bacteria irritate the kidney tissue, they trigger a whole‑body response. The main symptoms of a kidney infection include:
- Fever higher than 38°C / 100.4°F
- Chills or shaking
- Pain in the side, flank, or lower back, usually on one side
- Nausea or vomiting
- Extreme fatigue or feeling “wiped out”
- Painful urination (burning or stinging)
- Needing to pee often, including at night
- Cloudy, bad‑smelling, or bloody urine
Patients often say, “I felt like I had the flu and a UTI at the same time.” That mix strongly suggests pyelonephritis rather than a simple bladder problem.
How kidney infection symptoms differ from bladder infection symptoms
A plain bladder infection usually stays local. It causes:
- Burning with urination
- Urgency
- Needing to pee small amounts frequently
- Mild pressure in the lower belly
The differences that point toward a kidney infection instead:
- Fever and chills – rare with just a bladder infection
- Side or lower back pain under the ribs
- Nausea and vomiting
- Feeling acutely ill, not just annoyed by peeing symptoms
If you have a known UTI and then develop fever, flank pain, or vomiting, treat that as a red flag. Doctors read that pattern as a sign that the infection climbed to the kidneys.
Red flag signs of infection
Call emergency care or see a doctor immediately if you notice:
- Fever over 39°C / 102.2°F
- Confusion or trouble staying awake
- Fast breathing or racing heart
- Severe side or back pain that does not ease
- No ability to keep fluids down
These signs of infection suggest that bacteria already spread beyond the kidneys into the bloodstream. At that stage, infections can lead to sepsis, a life‑threatening condition that needs urgent hospital treatment.
4. Causes of kidney infection and who faces higher risk
The common cause: bacteria moving up
The direct causes of kidney infection center around bacteria, mainly E. coli. Research shows that E. coli causes up to 80 to 90 percent of uncomplicated UTIs and kidney infections in healthy women.[3]
How does it happen?
- Bacteria from the gut reach the urethra.
- They travel upward into the bladder.
- Without treatment, they climb the ureters and invade the kidneys.
That simple path explains why a kidney infection can start from something that looks harmless: burning when you pee.
Conditions that make it easier for bacteria to reach the kidneys
Certain medical problems make it easier for bacteria to travel and cause kidney infections:
- Kidney stone – stones block urine flow and give bacteria places to hide.
- Enlarged prostate in men – slows bladder emptying.
- Structural problems of the urinary tract present from birth.
- Long‑term urinary catheters.
- Prior urinary surgery.
When urine cannot flow freely, bacteria linger and multiply. That stagnant environment pushes a simple UTI toward the kidneys.
Chronic diseases that raise the stakes
Some chronic illnesses change how the body fights infection or how well kidneys work:
- Diabetes – weakens immune defenses and alters urine chemistry, both of which help bacteria.
- Chronic kidney disease – damaged kidneys clear bacteria less efficiently and sustain more harm from each infection.
- Long‑standing high blood pressure – injures kidney blood vessels and cuts reserve capacity.
- Any weakened immune system from conditions like HIV, cancer treatment, or immune‑suppressing drugs.
Experts report that people with diabetes face a significantly higher risk of both UTI and pyelonephritis, and they suffer more complications.[4] In these groups, a kidney infection can lead to scarring and permanent loss of function much faster.
Pregnancy and kidney infections
Pregnant women sit in a special risk category. The growing uterus presses on the ureters. Hormonal shifts relax the muscles of the urinary tract and slow urine flow. Both changes make it easier for bacteria to ascend.
Because of this, obstetric guidelines treat any signs that a pregnant woman may have a kidney infection as urgent.[5] Even a mild UTI gets prompt antibiotic treatment in pregnancy to shield both mother and baby from harm.
5. How kidney infections can lead to serious kidney damage
What happens inside the kidney
When bacteria invade kidney tissue:
- The immune system sends white blood cells to fight.
- Inflammation swells the tissue.
- The tiny filters and tubules that clear waste become damaged.
After a single severe infection, some people heal fully. Others develop patches of scar tissue in the kidney. Repeated attacks or one very severe episode increase scarring.
Over time, that scarring counts as kidney damage. Enough damage, and the kidneys cannot filter blood properly, which leads to chronic kidney disease.
From infection to kidney failure and sepsis
Serious infections can lead to:
- Loss of kidney function
- High blood pressure that becomes harder to control
- Anemia and bone problems from reduced kidney hormone activity
- Eventual kidney failure that requires dialysis or a kidney transplant
On top of that, because kidneys handle so much blood flow, bacteria can break out into the bloodstream. Doctors call this bacteremia or sepsis. Research shows that up to a quarter of adults admitted with severe pyelonephritis have some level of sepsis on arrival.[2]
That is why no doctor treats a kidney infection as “just another UTI.” A kidney infection can lead directly to intensive care when neglected.
6. How doctors diagnose a kidney infection
You might wonder, “How does a doctor know that this is a kidney infection and not just back strain or a flu plus UTI?” The process follows a clear, evidence‑based pattern.
1. Medical history
The clinician asks specific questions:
- When did your symptoms start
- Do you have burning or urgency when you pee
- Have you ever had a UTI or kidney infection before
- Do you have diabetes, kidney disease, or other chronic issues
- Are you pregnant
- Have you noticed blood in your urine
That history already separates kidney infection from many other causes of back pain.
2. Physical examination
The exam usually focuses on:
- Temperature, heart rate, and blood pressure
- Gentle tapping over the flanks and lower back
- Abdominal exam to detect tenderness or a full bladder
- Signs of dehydration or confusion
Sharp pain when the doctor taps over a kidney area strongly supports pyelonephritis.
3. Urine tests
The next step uses urine:
- Urinalysis – checks for white blood cells, red blood cells, nitrites, and bacteria.
- Urine culture – identifies the specific germ and tests which antibiotics kill it.
Urinalysis gives results in minutes. The culture takes one to three days but guides precise antibiotic choices, especially when the first drug does not work.
4. Blood tests and imaging
In more serious or unclear cases, doctors add:
- Blood tests to check kidney function, electrolytes, and infection markers.
- Blood cultures if they suspect bacteria in the bloodstream.
- Ultrasound or CT scans to look for stones, blockages, abscesses, or structural problems.
Imaging matters when a simple infection does not improve as expected, or when a stone or obstruction might block urine flow and cause kidney injury.
Distinguishing kidney infection from other problems
Doctors separate kidney infection from:
- Simple bladder infection – no flank pain or high fever.
- Muscular lower back strain – no urinary symptoms or fever.
- Kidney stone without infection – intense flank pain but clear urinalysis, no bacteria growth.
- Gynecologic issues in women, prostate problems in men.
That full workup, not just a symptom checklist, gives a confident diagnosis.
7. Treatment options: how to clear a kidney infection fast and safely
The central role of antibiotics
A true kidney infection never clears with cranberry juice, herbal teas, or home remedies alone. It needs an antibiotic chosen for the likely bacteria and your health situation.
Doctors decide between:
- Oral antibiotics at home – for stable patients who can drink fluids, with not too severe symptoms.
- Intravenous antibiotics in hospital – for high fever, vomiting, pregnancy, sepsis suspicion, or underlying chronic disease.
Common oral choices (depending on local resistance patterns) include fluoroquinolones or certain beta‑lactam antibiotics. Severe infections often start with IV drugs like ceftriaxone or piperacillin‑tazobactam, then step down to pills once the patient improves.
Research shows that a 7 to 14 day antibiotic course clears most straightforward kidney infections when people start treatment promptly and finish the full course.[2][3]
Why finishing the antibiotic course matters
Stopping antibiotics early invites relapse and resistance. Here is a typical pattern I see in case reports:
- Day 1–3: Patient starts antibiotics, fever falls, pain improves.
- Day 4–5: Patient feels “almost normal” and stops pills.
- Day 7–10: Symptoms roar back, sometimes worse, with more resistant bacteria.
Finishing the full course gives the immune system time to mop up remaining bacteria and helps prevent repeat infections.
Supportive home care that speeds recovery
Along with antibiotics, home care matters:
- Hydration – drink plenty of water unless your doctor imposes a fluid limit. Aim for clear or pale yellow urine.
- Rest – give your body time to focus on recovery.
- Pain and fever control – use paracetamol or doctor‑approved pain relief. Avoid anti‑inflammatory drugs like ibuprofen if your doctor warns about kidney strain.
- Light, frequent meals – ease nausea with small amounts of bland food.
If you cannot keep fluids down or you get more short of breath, dizzy, or confused, go back for urgent care. Those changes signal that home treatment no longer gives enough support.
Real‑world example
Here is a typical case pattern:
A 32‑year‑old woman with no prior kidney disease develops burning with urination and ignores it. Two days later, she spikes a 39°C fever, feels sharp pain on her right side, and vomits twice. In urgent care, her urinalysis shows heavy white cells and nitrites. The doctor diagnoses a right kidney infection and gives an IV dose of ceftriaxone, then a 10‑day oral antibiotic course.
She drinks water steadily, rests, and tracks her temperature. By day 3, her fever resolves. By day 7, her flank pain vanishes. She finishes all pills and sees her doctor once more. A repeat urine test returns clear, and she discusses prevention strategies to avoid a repeat.
8. Prevention: daily habits that help prevent kidney infections
You lower your risk of kidney infections by attacking the problem at its source: bladder infections and bacterial entry into the urinary tract.
Hydration and bathroom habits
Simple steps create powerful protection:
- Drink plenty of water during the day unless a doctor limits your fluids.
- Do not hold your urine for long periods. Empty your bladder every 3 to 4 hours while awake.
- Urinate right after sexual activity to flush bacteria from the urethral area.
- Avoid perfumed feminine hygiene sprays or harsh soaps around the genital region.
These habits keep urine moving and reduce how long bacteria sit in the bladder.
Hygiene: front to back really matters
To reduce contamination:
- After using the toilet, always wipe from front to back.
- Teach children the same front to back motion early.
- For those with limited mobility or needing caregiving, remind caregivers to wipe front to back as well.
This simple change cuts the chance that gut bacteria reach the urethra and get a kidney infection started.
Managing chronic conditions
Strong kidney protection goes beyond the urinary tract:
- Keep diabetes under tight control; high sugar levels feed bacteria and weaken immune defenses.
- Work with your doctor to keep high blood pressure in target range to protect kidney blood vessels.
- Monitor for chronic kidney disease progression with regular blood and urine tests if you already have reduced kidney function.
Experts suggest that stable blood sugar and blood pressure lower the risk that a kidney infection can lead to further damage in already vulnerable kidneys.[4]
Special guidance for pregnant women
If you are pregnant:
- Report any burning or urgency with urination early.
- Attend all prenatal visits, which often include urine checks.
- Follow every antibiotic prescription exactly as written if your doctor prescribes one.
Obstetric teams treat UTIs in pregnancy as serious for a reason. Fast treatment breaks the chain before an infection climbs.
9. When you must seek medical care immediately
You never wait and see with strong kidney infection signs. Call emergency services, go to an emergency department, or at least same‑day urgent care if you notice:
- Fever above 39°C / 102.2°F
- Shaking chills
- Severe side or lower back pain
- Vomiting that prevents you from keeping down fluids or pills
- Confusion, disorientation, or extreme sleepiness
- Chest pain, trouble breathing, or bluish lips or fingers
- No urine output for 8 hours despite drinking
These signals show that the infection already stresses the body, and delaying raises the risk that infections can lead to sepsis and kidney failure.
You also need prompt (same‑day or next‑day) care if:
- You have a UTI and new flank pain.
- You have diabetes, kidney disease, or a weakened immune system and develop UTI symptoms.
- You suspect your child or an elderly family member has a kidney infection.
- You started antibiotics for a UTI but get worse instead of better over 24 to 48 hours.
Fast action keeps a treatable infection from turning into a life‑threatening emergency.
10. Your step‑by‑step action plan if you think you may have a kidney infection
When someone worries that they may have a kidney infection, confusion sets in. Here is a clear workflow you can follow today.
Step 1. Check your main symptoms
Ask yourself:
- Do I have burning or urgency with urination
- Do I have fever or chills
- Do I have new one‑sided flank or lower back pain
- Do I feel acutely ill, not just mildly off
Any combination of urinary symptoms plus fever or flank pain deserves urgent evaluation.
Step 2. Call a health professional now
Explain clearly:
- “I have painful urination and now I have fever and side pain. I am worried about a kidney infection.”
This language immediately signals risk to triage nurses and doctors.
Step 3. Prepare for the visit
Bring:
- A list of medications and allergies.
- A brief timeline of symptoms.
- Any prior lab reports related to UTI or kidney issues.
If you live with chronic kidney disease, write down your most recent kidney function numbers if you have them.
Step 4. Follow through with tests and antibiotics
If your doctor orders urine tests or imaging, get them done. Start antibiotics as soon as prescribed. Set alarms on your phone so you never miss a dose.
Step 5. Monitor at home
Track:
- Temperature twice a day.
- Pain level in the side or back.
- Ability to drink and pee.
If your fever climbs again after falling, or if pain sharply worsens, contact your doctor or return to urgent care.
Step 6. Plan follow‑up and prevention
Once you recover, ask your clinician:
- What probably triggered this infection
- How to reduce the chance of another one
- Whether you need additional tests for stones or structural issues
That follow‑up keeps one crisis from turning into a long‑term pattern.
11. Key takeaways
- A kidney infection is a serious form of urinary tract infection that attacks the kidney tissue itself.
- Flu‑like illness plus UTI symptoms strongly suggests pyelonephritis, not a simple bladder infection.
- E. coli and similar bacteria make up the main common cause of these infections.
- Diabetes, kidney stone, chronic kidney disease, high blood pressure, pregnancy, and a weakened immune system increase both risk and severity.
- Untreated kidney infections can lead to kidney damage, scarring, sepsis, and kidney failure.
- Doctors diagnose with history, exam, urine tests, and sometimes imaging.
- The right antibiotic, started quickly and taken fully, cures most kidney infections before lasting harm occurs.
- Good hydration, bathroom habits, and wiping front to back help prevent future infections.
- Never ignore severe or fast‑worsening symptoms. Timely medical care protects you more than any home remedy.
People also ask
A true kidney infection does not clear reliably without antibiotics. The bacteria sit in an organ with rich blood flow, which lets them spread quickly. Without targeted treatment, the infection keeps damaging kidney tissue and can spill into the bloodstream. Supportive care like fluids helps, but it never replaces proper antibiotics.
Most people with an uncomplicated kidney infection start to feel better within 48 to 72 hours after the first antibiotic dose. Fever drops first, followed by less flank pain and improved energy. Full recovery, including normal stamina, takes one to two weeks. People with chronic illnesses, stones, or structural problems often need longer.
All kidney infections count as UTIs, but not all UTIs reach the kidneys. A standard UTI usually means a bladder infection, which stays low and causes mainly urinary symptoms. A kidney infection sits higher and causes systemic symptoms like fever, chills, and flank pain. Doctors take kidney infections more seriously because they carry higher risk.
Yes. Strong evidence shows that severe or repeated kidney infections scar the kidney tissue.[2] Enough scarring leads to chronic kidney disease and eventually kidney failure in some patients. The risk climbs when infections go untreated, treatment starts late, or the person already has reduced kidney function.
Women face higher risk because of their shorter urethra and anatomy. People most likely to get kidney infection complications include those with diabetes, chronic kidney disease, kidney stones, urinary tract blockages, pregnancy, and those with a suppressed immune system. For these groups, doctors keep a lower threshold for doing tests and starting antibiotics early.
References
- National Institute of Diabetes and Digestive and Kidney Diseases. Urinary Tract Infection in Adults. niddk.nih.gov
- Talan DA, et al. “Acute pyelonephritis in adults.” New England Journal of Medicine.
- Gupta K, et al. “International clinical practice guidelines for the treatment of acute uncomplicated cystitis and pyelonephritis.” Clinical Infectious Diseases.
- Nitzan O, et al. “Urinary tract infections in patients with type 2 diabetes mellitus: review of prevalence, diagnosis, and management.” Diabetes, Metabolic Syndrome and Obesity.
- American College of Obstetricians and Gynecologists. Practice Bulletin on Urinary Tract Infections in Pregnancy.
(References listed for educational purposes; readers should check the latest local and international guidelines for up‑to‑date details.)
Author bio
Author: Dr Adam Khan
Dr. Adam focuses on kidney and metabolic health, with a special interest in preventing infections and protecting long‑term kidney function. He combines current clinical research with practical advice that patients can apply in daily life.